Melanoma is known as the most serious form of skin cancer. Through early detection and intervention, however, you can receive effective treatment and potentially make a full recovery. In Delray Beach, FL, you can rely on Feinstein Dermatology as a trusted name in skin cancer care and melanoma diagnosis and care.
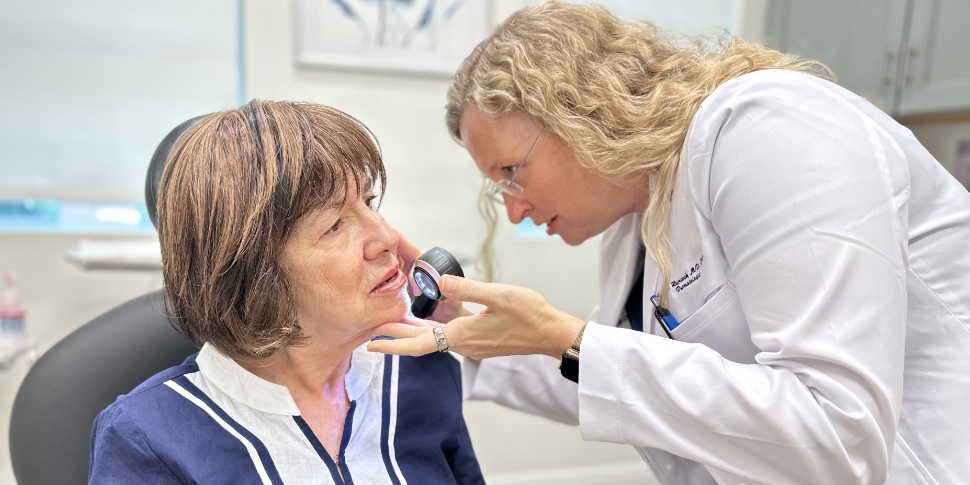
What Is Melanoma?
Melanoma is a type of skin cancer that develops in the cells that produce melanin. These are known as the melanocytes. Though less common, melanoma may also form in your eyes or internal organs. While melanoma can occur anywhere on the body, it is especially common in areas with frequent sun exposure. You can typically detect melanoma via the change in appearance of an existing mole or the development of a new pigmented area on your skin. It’s important to note an increased risk if a family member has had melanoma or if you have numerous moles on their skin.
What Are the Causes of Melanoma?
Although we don’t fully understand the precise cause of melanoma, it is widely perceived to result from exposure to UV rays through direct sunlight or tanning beds. Melanoma can affect men and women of all ages, and in fact, it is becoming more and more common among those under the age of 40. It is critical for you to know the warning signs of melanoma and to seek assessment and diagnosis as promptly as possible.
Melanoma Treatment
Your treatment journey will begin with a careful diagnosis. Your board-certified dermatologist can sometimes confirm the presence of skin cancer with merely an external evaluation, but an accurate diagnosis requires a biopsy. Following the biopsy, your dermatologist will determine the thickness of the melanoma and assess its spread throughout the body. Treatment usually involves the removal of the melanoma and a wide excision of the surrounding skin, followed by aesthetic repair.
Biopsy procedures used to diagnose melanoma include:
- Punch biopsy. During a punch biopsy, your doctor uses a tool with a circular blade. The blade is pressed into the skin around a suspicious mole and a round piece of skin is removed.
- Excisional biopsy. In this procedure, the entire mole or growth is removed along with a small border of normal-appearing skin.
- Incisional biopsy. With an incisional biopsy, only the most irregular part of a mole or growth is taken for laboratory analysis.
The type of skin biopsy procedure you undergo will depend on your situation.
Tips for Managing Melanoma
The best thing you can do to minimize your melanoma risk is to practice sun safety by wearing proper protection all year long. Regular skin examinations, including both professional and self-evaluations, are also critical for early detection.
Melanoma FAQ
Meet Our Board-Certified Dermatology Team
At Feinstein Dermatology in Delray Beach, FL, our commitment is patient satisfaction and loyalty. We are defining the new standard in customer experience and outcomes, striving to lead by example for others to follow. With a dedicated patient base of over thirty-five thousand (35,000) individuals who have entrusted us with their dermatological and cosmetic needs, we have earned our reputation as a leading provider in the field.
Our team comprises dedicated professionals, including board-certified dermatologists, a board-certified Mohs surgeon, and a board-certified plastic and reconstructive surgeon. We invite you to experience the exceptional care and dedication that defines Feinstein Dermatology.
LEADERS IN DERMATOLOGY & COSMETICS
Meet Your Providers
Feel Good About Your Skin
At Feinstein Dermatology & Cosmetic Surgery, we understand that your skin is more than just an organ; it reflects your well-being and confidence. Our dedicated team of board-certified dermatologists and skincare specialists is committed to guiding you on a transformative journey toward feeling fantastic in your own skin. With a personalized approach to dermatological and cosmetic care, we aspire to be your trusted partners for a lifetime of radiant, healthy skin. Take the next step towards embracing your confidence with advanced skincare solutions, cosmetic care, or skin cancer treatments in Delray Beach, FL. Schedule a consultation for melanoma treatment today at (561) 498-4407.